![]() What is a Varicose Vein?
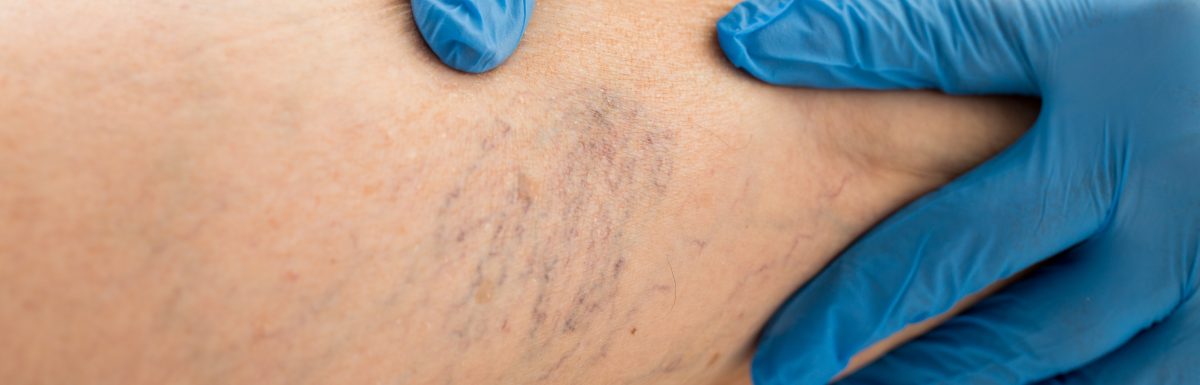
What is a Varicose Vein?
A varicose vein describes a buildup of blood inside a small blood vessel causing it to swell and twist. It eventually becomes visible just under the skin.
The body is full of veins carrying deoxygenated blood from tissues back to the heart. If one suffers damage or becomes weak, it is unable to transport blood from the lower body to the heart. Since it is a one-way channel, its content will pool inside, prompting swelling.
It is typically seen in the elderly, pregnant women and those who are overweight or suffer from obesity. It might occur following prolonged periods of inactivity or trauma. (1)
Symptoms
Superficial veins are located just under the skin. These extract “used” blood and transport it to a deeper tube which will bring it back to the heart.
Inside each vein there are small flaps (valves) which keep the blood flowing in one direction. These open and close to allow an upward stream to the heart. (2)
However, if these fail to work the blood will pool, creating a build up in the superficial vein. Eventually, the channel will swell, harden and appear lumpy as the tube twists and turns.
A varicose vein can develop anywhere, but it is more commonly seen around the legs. This is a vulnerable place as the vessels must pump upward against gravity’s pull.
It’s a condition which does not have many symptoms and fortunately, it will not always cause medical complications.
Symptoms can include the following:
Visible Veins
This is a telltale sign of a varicose vein.
When the wall of the vein becomes weak, it will cause the valves to lose their elasticity, hindering them from closing. The blood will run backwards toward the legs until it encounters a working flap. (3)
Here it will cause a buildup which eventually expands the vein, causing it to appear larger and more apparent from the outside. This gives rise to the typical characteristics of a varicose vein.
Swelling
The blood falls back towards the leg due to gravity’s pull. The pressure will force the surrounding fluids to leak out into tissues, causing them to swell.
A hallmark swelling from varicose veins occurs around the ankles and calves. The feet will usually remain somewhat unaffected.
It is often worse during the day after standing up or walking around. However, in the morning it might not be noticeable. (4)
Pain
When buildup and swelling occur, they can cause discomfort in the legs.
Those affected might describe it as “heavy legs.” Some might perceive this as mild achiness, while for others it can be quite painful. Cramping and a feeling of throbbing may also become apparent. (5)
This symptom seems to be very prevalent for women during pregnancy, where pain might be felt in a sequence with numbness and cramps. This also may become more evident at night. (6)
Itchy Skin
A varicose vein is likely to cause the skin on the affected area to itch.
It can be due to swelling which causes the skin to tighten and may eventually result in itching. This symptom can be misleading, as it is often misdiagnosed as dry skin. (7)
Appearance
When a vein becomes larger and more apparent, it is likely to change the appearance of the skin. (8)
The skin’s exterior may become lumpy due to small blood clots inside. When more substantial amounts build up, it can change the color, and the area might appear dark, almost purple or blue.
Stages
A varicose vein is classified into eight stages. The classification system is called clinical etiology anatomy pathology (CEAP). It describes the severity of symptoms to help doctors prescribe treatment. (9, 10)
A varicose vein stems from a condition called venous reflux. This disease can occur in deeper veins or superficial ones closer to the surface.
Usually, a varicose vein is an indicator of deep venous reflux. The staging has been laid out to describe progression from mild symptoms to severe, which might be in need of urgent treatment.
Stage #0 (C0)
The patient is not yet diagnosed but can be seen complaining about several symptoms which could indicate a varicose vein. This could include heaviness in the legs, swelling or achiness and night cramps. However, these are very common so at this point may not be identified as signs of a varicose vein.
Stage #1 (C1)
During this stage veins might appear broken or tangled.
This condition is not yet labeled as a varicose vein, but instead as telangiectasia, which describes tangled veins. These are sometimes referred to as spider veins.
Stage #2 (C2)
If the blood vessels begin to bulge outwards when the affected stands, the patient will be diagnosed with a varicose vein.
Stage #3 (C3)
When the varicose vein give rise to swelling, the patient will show a progression to stage C3.
As we established earlier, this swelling mostly affects the ankles and around the calves, but it will generally leave the feet unaffected.
Stage #4A (C4A)
The patient’s skin around the affected area begins to change its appearance to a darker color. Some might experience an eczema-like rash which may cause itching.
Stage #4B (C4B)
This stage is classified as lipodermatosclerosis and atrophie blanche, which are two conditions that may indicate damaged skin.
The first describes redness or a darker color afflicting the lower leg, right around the calves and ankles. The second can be characterized by white spots usually following an injury to the skin which keeps the blood from flowing.
Stage #5 (C5)
This stage can seem illogical in the sequence, as the damages to the surface will begin to heal.
Stage #6 (C6)
Poor circulation is starting to show its effect. Sores or ulcers are beginning to reappear on the leg.
This indicates the most severe stage where the ulcer will be active. It’s likely infected by bacteria and may cause complications.
Treatment
Treatment of a varicose vein revolves around lifestyle changes and surgical procedures. (11)
Unless the condition causes severe symptoms and appears bothersome, doctors might only prescribe a healthy lifestyle change. However, some people might feel insecure about the appearance of the veins and may prefer a cosmetic procedure to correct this.
Lifestyle Changes
Lifestyle changes might include maintaining a healthy weight, staying active and avoiding sitting or lying down too much. (12)
Increased muscle strength in the legs is an excellent way to improve blood flow. Wear sensible shoes as often as you can. Footwear with a flat heel can help build muscle strength.
Avoid wearing tight clothing, especially jeans or trousers, as much as possible. These could tighten circulation even further.
Talk to your doctor about compression socks. These might also help with circulation, especially in situations where you are required to sit or stand for prolonged periods. (13)
Sclerotherapy
This treatment is used to close off a vein. It involves injecting a specific chemical substance into the area where it will cause scars and irritation. Eventually, it will close entirely and will not be visible. (14)
Laser Surgery
Laser surgery is used to fade the vein. During the procedure, the doctor will use a beam of light to dissolve the blood vessel so it won’t be as noticeable. (15)
Endoscopic Vein Surgery
This procedure is only used in severe cases. It involves an incision into the leg where a small device guided by a camera is inserted. This allows the doctor to close the vein. (16)
Ambulatory Phlebectomy
If the varicose vein is close to the surface, your doctor might prefer to remove it. A small incision is made in the skin and the offender is removed. (17)
Vein Stripping and Ligation
Amputation of the vein is usually only done in severe cases. The surgeon will make cuts along the leg and extract the blood vessel. This procedure is carried out whilst you are unconscious and recovery may take longer. (18)
FAQ
What is a varicose vein? A varicose vein is a swollen, lumpy blood vessel which can be seen through the skin.
What are the signs of a varicose vein? In mild cases, noticeable veins and mild swelling might be the only indicators. As the condition progresses other symptoms can include pain or achiness, a “heavy leg,” itchy skin and dark patches or threads along the legs.
How do you develop a varicose vein? It develops when the vein’s ability to pump blood up towards the heart is compromised. This may occur following prolonged periods of inactivity or when excessive weight is put on the legs, including pregnancy or obesity.
How are you diagnosed for a varicose vein? Diagnosis can be done by a physical examination and information about the symptoms. Additional testing can include a duplex ultrasound which will check the blood flow. (19)
What is the best treatment of a varicose vein? In some cases, a healthy lifestyle may help solve the problem. Otherwise, treatment can involve different medical procedures which will work to close the vein or remove it entirely.
What are the long term complications of a varicose vein? A varicose vein rarely leads to any serious medical complications. But it’s important to look out for signs of progression, such as ulcers, extreme swelling or excessive bleeding under the skin. (20)
Is a varicose vein considered a disability? A varicose vein is not considered to be a disability.
Is there any cure for a varicose vein? The affected vein can be removed with surgery and symptoms can improve with changes to a more active lifestyle.
Is a varicose life threatening? A varicose vein on its own is generally not life threatening.
Summary
A varicose vein is a visible, lumpy blood vessel caused by an impairment in the valves which help the blood flow from the legs toward the heart.
When the small valves inside the vein suffer damage, the blood will run back to the legs, creating a buildup. This will cause the vein to swell and twist, giving rise to this condition.
It is typically nothing serious and may be easily treated with an active lifestyle and minor procedures.