![]() What is Ringworm?
What is Ringworm?
Ringworm is a type of skin infection caused by a fungus. It is defined by a circular rash which can appear anywhere on the skin.
Ringworm remains a widespread fungus, as it readily transmits from one person to another upon contact. It may also spread from animals and contaminated objects such as fabrics, moist surfaces or household equipment. (1)
The ringworm fungi thrive best in moist, warm environments, such as the groin area, feet or underneath a thick beard. These are generally covered, trapping the moisture inside.
Symptoms
The name ringworm is believed to be based on its trailing border. It might resemble tracks or threads from a creeping worm snaking its way around the skin. (2)
Even though the name might suggest it, a ringworm rash is not caused by a worm living inside the body. As mentioned above, the culprit is a fungus. These are a normal part of everyday life, and a person often inhales spores on a daily basis. (3)
Ringworm has an ability to live on the surface without causing any noticeable signs. However, as soon as a break in the skin occurs, it will multiply and invade the tissue.
The rash can be characterized by a scaly, raised border around a circular red blemish. These can vary in size, but typically start out as a small spot and will proceed to grow, unless treated. (4)
Ringworm can spread very quickly upon slight contact. Those suffering from a weak immune system or a disease compromising its functions, such as AIDS, may find it harder to fight. (5)
A ringworm infection can present with a variety of names. These will depend on the location of the rash. Commonly known terms can include athlete’s foot or jock itch.
Signs may also differ depending on the location. Below is an explanation of symptoms as they develop on the different body parts.
Body
Ringworm on the body will generally manifest with the hallmark of this fungus; a ring-shaped border that is trailing around a red, itchy rash. (6)
The ring usually starts out around a tiny center, and slowly increases in size. The border will appear red or pink on lighter skin tones, and purple or brown on darker skin. It is likely to have a dry texture and is slightly raised above the center, creating a crater-like dent.
Patches of ringworm tend to become profoundly itchy and will usually seem dry and flaky.
Feet (Athlete’s Foot)
Generally, if the rash is affecting the feet, dry scaly skin may begin to manifest between the toes, where it might proceed to spread. The affected may not encounter the same ring-shape, as the rash has a tendency to spread outwards rather quickly. (7)
The surface of the feet can begin to peel off leaving a very painful area where blisters can develop. The feet may then become prone to cracking. This may result in bleeding followed by thick patches of skin.
Those affected might also experience a soft, mushy texture on the feet, specifically between the toes. This could present with a foul smell.
Hands
The hands, especially the palms, are particularly prone to ringworm infections. They are often used to scratch and examine rashes in other locations, exposing them to the fungus. (8)
When the palms are affected, the rash will generally exhibit a widespread area of red, dry, flaky skin that quickly covers most of the surface.
Circular-shaped patches are likely to develop on the back of the hand and can be very itchy.
Nails
When ringworm spreads to the nails on either fingers or toes, it will generally begin at the nail bed. The skin will thicken, and nails are likely to change color. (9)
Thickening of the nails may also become more apparent. They may begin to lift away from the bed, and over time they could start to crumble and disappear entirely.
Groin (Jock Itch)
An early sign of a jock itch is a red swollen rash that is very itchy, located in the crease where leg and body meet. It will slowly spread to the groin area before reaching the inner thighs, waist and buttocks. The skin may appear dry and flaky with a raised border. (10)
Scalp and Beard
If the ringworm has infected the scalp or beard area, the affected is very likely to experience hair loss. (11)
Those affected will usually exhibit a growing bald spot with thick, patchy skin. Small black dots may become visible around the area, which is likely to itch.
Acne-like spots may develop which can rupture and leak, as well as open sores seeping pus.
Stages
The medical term for ringworm is dermatophytosis. This type of fungus can be described through different stages of its invasion of the human body. Most people will generally not progress to the last stages, except those who have a weakened immune system. (12)
Stage #1 (Adherence)
After the fungus has entered the skin, it must find a way to reproduce and begin its invasion. Ringworm carries asexual spores which need to attach to keratin cells in the skin tissue.
When they are near the skin’s surface, long thin threads of fiber help connect the fungus and keratin. However, for the spores deeper in the skin, they must form a “sticky” exterior to connect with other cells and multiply.
Stage #2 (Penetration)
The ringworm needs a way to get through to the deeper tissues. In order to do this, it will establish an army of tiny fighters, which will break down the body’s natural proteins. The fungus can now enter the next layer of skin before being eliminated when the outer layer sheds.
Stage #3 (Host Responses)
During this stage, the body will begin to react to the invasion. As the ringworm is spreading, it will cause profound redness, itching and acne-like formations.
In patients with a functional immune system, signals to the brain will be sent requesting that antibodies are launched. However, those with a compromised defense may progress to the next stage at a more intense rate.
Stage #4 (Acquired Resistance)
The immune system is launching its response which may cause mild to severe inflammatory symptoms. The severity will depend on the status of the patient and type of ringworm.
Stage #5 (Antibodies)
In stage five the antibodies show little to no effect on the invasion. The fungus is now traveling to the nearby lymph nodes where it will cause more severe inflammatory responses.
Stage #6 (Hypersensitivity)
The patient may exhibit eczema-like reactions as a response to the inflammation. However, these may appear further away from the site of infection.
Stage #7 (Non-Specific Resistance)
The body requires a functional immune system to be able to fight off the invasion. Patients with a weakened defense are likely to progress to the last stage.
Stage #8 (Invasive Dermatophytosis)
In the last stage, the ringworm will penetrate through to the deeper layers of the skin. Here it can develop ulcers which may bleed and spread the fungus further.
This stage will usually only affect those who have a weak immune system.
Treatment
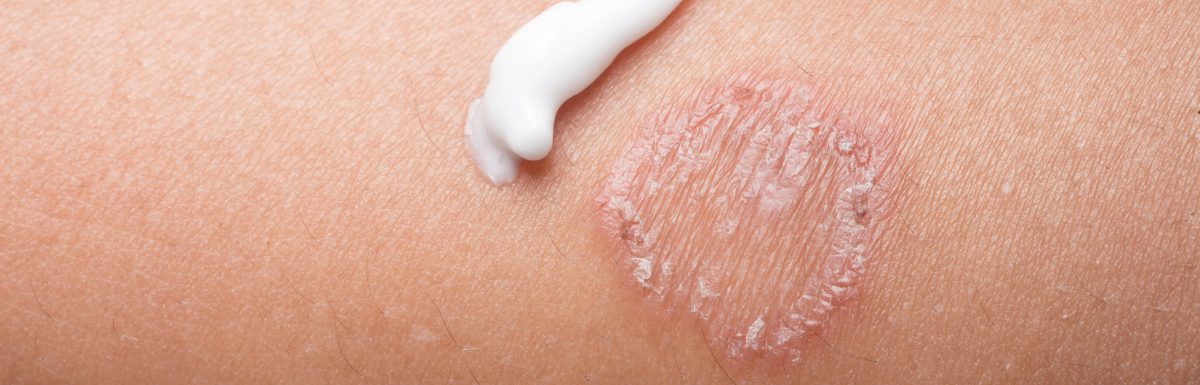
Treatment of ringworm will often revolve around antifungal medications. These will be prescribed depending on the location and the severity. (13)
In many cases, doctors will recommend using a topical cream. These are usually applied twice a day for a few weeks until symptoms subside.
Many of these are very safe to use and will work efficiently, even for children. It is, however, essential to finish the dose to ensure complete elimination of the ringworm. This may take up to two weeks.
When the ringworm has affected larger areas or more complicated places, such as the scalp or groin, prescription medication is typically needed.
If ringworm is affecting skin underneath a beard the affected is likely to be asked to shave. A dermatologist may then proceed to remove parts of the affected tissue. (14)
FAQ
What is ringworm? Ringworm is a specific type of fungus causing circular-shaped rashes.
What are the signs of ringworm? Symptoms depend on location. The infection generally manifests with red patches surrounded by a dry and scaly, slightly raised border. It will usually cause significant itching which may lead to burning, sometimes painful sensations.
How do you develop ringworm? Traits of ringworm are typically always present on the skin. When a slight break in the surface occurs, it will seep inside and begin invasion. It can transmit from person-to-person, but it can also survive on floors or objects. Animals and pets have shown to be prominent carriers. (15)
How are you diagnosed for ringworm? Its signs are very distinguishable, so a dermatologist will generally examine the skin and make a diagnosis from there. Sometimes a sample might be sent to a lab for a closer look. (16)
What is the best treatment for ringworm? The primary treatment is antifungal medication. These may involve creams or oral pills. If the fungus affects the scalp, it might need a special shampoo. (17)
What are the long term complications of ringworm? The ringworm may reinfect healed tissues, so preventative measures should be taken. For those with a weak immune system, the infection could lead to complications. The body will find it harder to defend itself and medication might not be as effective. The skin might be left vulnerable to other opportunistic diseases. (18)
Is ringworm considered a disability? No, ringworm is not a disability.
Is there any cure for ringworm? The fungus can be eliminated with treatment.
Is ringworm life threatening? Ringworm is not life threatening, but it can leave immunosuppressive individuals vulnerable to other diseases and infections. (19)
Summary
Ringworm is a fungus affecting the skin. It causes a unique rash, characterized by a raised, circular border trailing a red itchy blemish.
It is very common and spreads rather quickly upon contact with the fungus if there’s a break in the skin. Many people may know it as jock itch or athlete’s foot.
Ringworm is very treatable with antifungal medication and cream. It can, however, be prevented by wearing shoes in public showers, washing hands after contact with animals and keeping skin dry and clean. (20)